If your child’s asthma suddenly get much worse (asthma attack), they will require urgent treatment. Signs of an asthma attack include:
- Being very wheezy
- Having a tight chest
- Finding it hard to breathe
- Being too breathless to speak is a sign of a severe asthma attack and needs emergency treatment
Looking after your child during an asthma attack
Sometimes there is no obvious cause for your child’s asthma attack, but the most common triggers are viral infections (coughs, colds and chest infections), sudden changes in the weather and exposure to cigarette smoke.
If you are concerned about your child’s symptoms please see the table below.
When should you worry?
If your child is:
- Too breathless to talk / eat or drink
- Has blue lips
- Having symptoms of cough/wheeze or breathlessness which are getting worse despite 10 puffs blue (salbutamol) inhaler every 4 hours
- Confused and drowsy
Ring 999 immediately for help. Give 10 puffs of blue (salbutamol) reliever inhaler every 10 minutes until ambulance arrives
Keep child in upright position and reassure them
If your child is:
- Wheezing and breathless and blue (salbutamol) reliever inhaler 2-5 puffs is not lasting 4 hours
- Having a cough or wheeze/tight chest during the day and night
- Too breathless to run / play / do normal activities
Immediately contact your GP and make an appointment for your child to be seen that day face to face
Increase blue (salbutamol) reliever inhaler 6-10 puffs every 4 hours
If symptoms persist for 4 hours or more and you have not been able to speak to either a member of staff from your GP practice or to NHS 111 staff, then consider taking them to your nearest Emergency Department
If your child starts to cough, wheeze or has a tight chest but can continue day to day activities
Give 2-5 puffs blue (salbutamol) reliever inhaler every 4 hours until symptoms improve
Information to help the health professional - substance:
- What substance did your child swallow or touch?
- When did this happen? How long ago?
- How did they come into contact with it? Did they swallow, breathe it in, lick it, etc.?
- How much of the substance was taken?
Information to help the health professional – your child:
- How old is your child and what is their estimated weight?
- Do they have any existing medical conditions?
- Are they taking any medications or treatments?
- Do they have any allergies?
What to do after seeking advice or being discharged from the hospital:
- Monitor your child for the next 1-2 days.
- Let them eat or drink normally.
- Follow the steps above if you are concerned about your child.
- Read the “Prevention is Better Than Cure” advice below.
What can you do to reduce the risk of your child having another asthma attack?
1) Children with poorly controlled asthma are much more likely to have an asthma attack compared to children whose asthma is well controlled.
Signs of poorly controlled asthma include your child having a regular cough at night (nocturnal cough), being wheezy or more breathless than other children when they run around (exertional dyspnoea) or using their reliever inhaler more often than expected.
Arrange to see your GP or asthma nurse if they are experiencing such symptoms.
To watch a video on encouraging children to use their inhalers effectively please click here.
2) It is vital that your child uses their inhalers correctly.
Your child’s asthma will not be controlled if their medicines are not getting into their lungs.
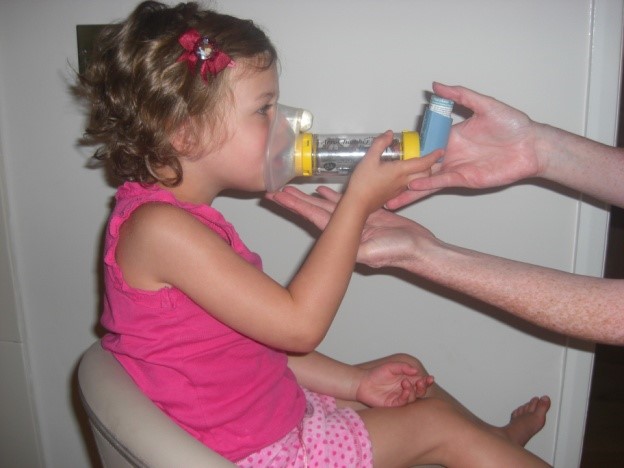
Choose appropriate sized spacer with mask (or mouthpiece if child is over 3 years with good technique and is not significantly short of breath).
- Shake the inhaler well and remove cap
- Fit the inhaler into the opening at the end of the spacer
- Place mask over the child's face or mouthpiece in their mouth ensuring a good seal
- Press the inhaler once and allow the child to take 5 slow breaths or slow count to 10 between ease dose
- Remove the inhaler and shake between every puff. Wait 1 minute between puffs

Repeat steps 1-5 for subsequent doses.
Plastic spacers should be washed before 1st use and every month as per manufacturer's guidelines.
For videos on using your child's inhaler and spacer correctly see goo.gl/235DQ 
See your practice nurse or doctor if you are not sure whether your child is using their inhaler properly.
3) Avoid triggers where possible:
Although it is extremely difficult to avoid your child getting a viral infection or experiencing changes in the weather, you can reduce exposure to common irritants such as cigarette smoke. Even where adults smoke away from their children, smoke on their clothes and hair is likely to make their child’s asthma worse.
4) Your child should have an influenza immunisation every autumn (the flu jab).
Not only can flu trigger an asthma attack in your child, your child is more likely to experience severe influenza if they have asthma. Protect them by having them vaccinated every year
What should you do?
At the start of cold symptoms (such as runny nose), begin your child on blue (salbutamol) reliever inhaler 2 puffs 4 hourly (including through the night). This can be increased to up to 10 puffs at a time if your child’s symptoms are still significant. If your child is requiring increasing amounts of blue inhaler you should seek medical advice according to the table below.
Treatment over the next few days
Over the next few days, you should follow the instructions on your child's personalised asthma action plan completed by their clinician. A template can be found here.
Where should you seek help?
- If it is non-urgent, speak to your local pharmacist or health visitor.
- If your child has any of the above features, urgently see your GP. For an urgent out-of-hours GP appointment, call NHS 111.
- You should only call 999 or go your nearest A&E department in critical or life threatening situations.
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns or to the Community Paediatricians or to the child and adolescent mental health services.
Contact them by phoning your Health Visitor Team or local Children’s Centre.
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information watch the video: What does a health visitor do?
School nurses care for children and young people, aged 5-19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and/or emotional health needs.
Primary and secondary schools have an allocated school nurse – telephone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:-
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
A&E departments provide vital care for life-threatening emergencies, such as loss of consciousness, suspected heart attacks, breathing difficulties, or severe bleeding that cannot be stopped. If you’re not sure it’s an emergency, call 111 for advice.



